We've joined our RTI Health Solutions colleagues under the RTI Health Solutions brand to offer an expanded set of research and consulting services.
The Mental Health Of Children & Young Adults: Effects Of The Pandemic
Much has been written about the overwhelming negative effect of the COVID-19 pandemic on mental health. However, its impact exacerbated an existing, decade-long trajectory toward a crisis in child and youth mental health. Conversely, some aspects of the pandemic yielded insights and glimmers of hope as to where healthcare must focus its efforts to support happier, healthier, more resilient young people.
Child and adolescent mental health before the pandemic
Statistics reveal informative patterns, but behind every number or data point is the life of a child or young person. When the U.S. Surgeon General issued an advisory to address the nation's youth mental health crisis in 2021, it was on the heels of a decade (2009-2019) of erosion of this vulnerable group as indicated in Figure 1.

Figure 1: Child and adolescent mental health indicators
Sources: KFF analysis, Washington Post, US Dept. of Health and Human Services
As the US headed into the pandemic, mental health challenges were already the leading cause of disability and poor outcomes in young people. Disturbingly, by 2018, suicide had become the second highest cause of death for young people ages 10 to 24.
Creating the COVID generation
Some have called the exacerbation of the existing mental health crisis for young people the epidemic within a pandemic.
Many aspects of the pandemic threw children and adolescents, along with their parents, teachers, caregivers, and pediatricians, into uncharted territory.


Figure 2: How the COVID-19 pandemic effected child and adolescent mental health negatively.
Sources: American Academy of Pediatrics (AAP), American Psychological Association (APA), KFF COVID-19 Vaccine Monitor, Centers for Disease Control and Prevention (CDC), UCSF, The Children's Hospital of Philadelphia (CHOP)
The perfect storm for emotional and psychological disease
The pandemic created untoward affects that brought about new mental conditions for children and adolescents, as well as exacerbated existing challenges. Four particular challenges have made the pandemic a more intense and multi-variate stressor for youth.
Social isolation and routine
The pandemic created disruptions to routines and social isolation for children.
KFF research revealed that relationships with their friends are relatively worse off since the pandemic began, impacting how young people interact with each other, as well as how they feel about those changes. Twenty-nine percent of children and adolescents reported that their relationships with families and friends had worsened.
Brian Jenssen, MD, MSHP, a primary care pediatrician in the Division of General Pediatrics at CHOP, along with colleagues from The Possibilities Project at CHOP conducted the study. He highlights the critical importance of routine, “There are three main treatment options for mental health-related conditions, and most people know about two: medication and counseling. But one treatment that many forget the importance of is routine. This pandemic pulled routine away from a vast majority of adolescents, which likely had a profound effect on them."
Greater impact to children from historically under-resourced families and communities
Isolation and being cut off from community and school-based services, such as early care and education, negatively impacted the emotional health of children from lower resourced homes.
Data shows the pandemic added to existing inequities for children receiving supportive programming for emotional, educational and behavioral health needs. Asian and Latino youth endorsed the "highest levels of feeling disconnected from school and poorer emotional and cognitive health."
From an HHS report: "Several studies found that children (age zero to five) from lower income households, single-parent families, and Black households, as well as young children with disabilities, experienced the largest increases in emotional or behavior problems, including depression."
Grief from loss
KFF analysis revealed that, as of June 2022, over 200,000 children in the US had lost one or both parents to COVID-19. And even a larger number has lost a grandparent or great-grandparent. The pandemic is estimated to have increased the number of bereaved children by 17.5%-20%. Corresponding to the disparities in death rates, children of color were more likely to lose of a parent, grandparent, or family caregiver.
Quoted in an APA article, Irwin Sandler, PhD, professor emeritus and research professor at Arizona State University (ASU) has studied childhood grief for over 30 years, sharing that about 20% of children “experience serious long-term problems, including long-term development of depression and long-term higher risk of suicide."
Children who have unaddressed grief and loss become adults who face increased risk for chronic illnesses, lower quality of life, and physical-mental co-morbidities.
Increased child abuse
The pandemic could become an adverse childhood experience (ACE) for many children and youth. This is particularly salient when considering those who live in unstable situations and adults have new pressures and uncertainties with the pandemic. One study found that 55% of children and youth reported emotional abuse by a parent or other adult in the home, including swearing at, insulting, or putting down the student. Another 11% experienced physical abuse by a parent or other adult in the home, including hitting, beating, kicking, or physically hurting the student.
Conversely, other studies concluded that there has been less abuse in the home during the pandemic. According to the CDC, 1 in 7 children experienced child abuse or neglect in 2019. One study followed 10,000 emergency room visits, finding that the “encounter rate for physical abuse diagnoses overall among all ages, per day, decreased by 19% during the pandemic." However, this same decrease was not seen in children under two or older than 13.
Some bright spots emerged from the pandemic
Research and surveys have also revealed some positive outcomes for child and adolescent mental health during the pandemic. A FiveThirtyEight and Ipsos survey, conducted in November 2021 with 1,000 young people and 1,500+ parents, found that “America's kids aren't as downtrodden as they're often made out to be." The parents were a likelier to report poor mental health, at 11%, compared to eight percent of teens. In fact, 96% of children ages 5 to 11 said that they felt very or somewhat good.
While 34% of parents were concerned about their kids' mental health, only 18% of teens were concerned about their own. In fact, about 50% thought that their mental health hadn't changed at all since the start of the pandemic and 20% thought their mental health had improved. As shown in Figure 3, there are a number of positive findings related to child and youth mental health during the pandemic.
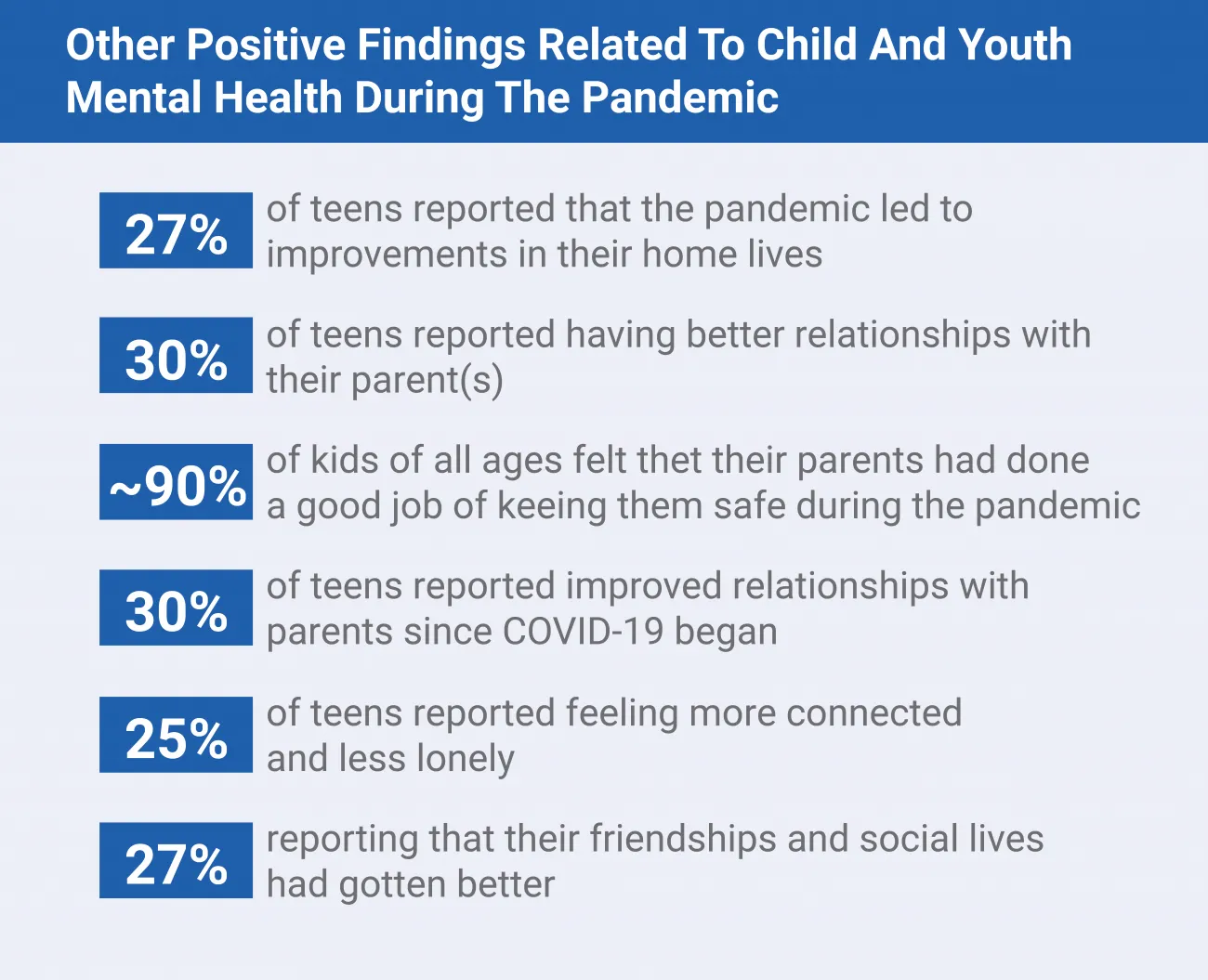
Figure 3: How the COVID-19 pandemic effected child and youth mental health in positive ways.
Sources: FiveThirtyEight and Ipsos
Children of color and differences in pandemic impact
Anna Gassman-Pines, a professor of psychology and public policy at Duke University, has led research on the impact of COVID-19 on families experiencing lower incomes, particularly with members working in the service industry. “There's a lot of good developmental science behind the idea that ultimately kids will be resilient," she said.
Her research, included in Figure 3, found that many positives remained when stratified by income and race. However, the research showed some disparities. “Black parents were more likely than White parents to report that they were concerned about their personal finances, and low-income parents reported worse finances and physical health than higher-income parents."
Yet, the number of teens who felt good about their home lives, relationships with parents, and mental health were quite consistent across income levels and race. Dr. Gassman-Pines found that, even when parents were facing challenges and their children were worried, the children didn't fare worse than others whose families didn't face the same challenges with income or job loss.
Supporting children and young adults into a post-COVID world
Children continue to re-assimilate into routines, but different from before the pandemic. In-person classes have resumed, many community activities have returned and yet there are still risks to children and youth, particularly with this winter's rise in advanced respiratory syndrome. Many children will develop new resiliency capabilities through the last few years while others will struggle with the permanent loss that they suffered. Healthcare will continue to research, assess, and find new ways to support children as they process, remember, and grow.
Population health, data science, and digital health work hand-in-hand
RTI Health Advance offers expertise across numerous disciplines to help healthcare organizations use the power of data to assess changes and trends in population health and create programs and tools to deliver high-quality care. Contact us.
Subscribe Now
Stay up-to-date on our latest thinking. Subscribe to receive blog updates via email.
By submitting this form, I consent to use of my personal information in accordance with the Privacy Policy.