We've joined our RTI Health Solutions colleagues under the RTI Health Solutions brand to offer an expanded set of research and consulting services.
Diabetes Population Health Strategies For Better Access To Care
Improving access to care: Everyone wins when diabetes risk factors are addressed
Diabetes continues to extend its reach deeper into the American population, with nearly one in three adults now living with the disease, twice the number of just 20 years ago. Another 84 million people have prediabetes, a condition which can lead to Type 2 diabetes within five years if left untreated.
Diabetes is costly
Type 2 diabetes accounts for about 95% of diabetes cases. It’s the seventh-leading cause of death in the U.S., resulting in annual care and treatment expenses of $327 billion. That’s about one-third of the $1.1 trillion the country spends annually on chronic diseases.
Entrenched health inequities in diabetes access to care
As with many other chronic illnesses, systemic inequalities leave some population groups at substantially higher risk for diabetes. A disproportionate number of those afflicted live in historically disinvested communities, have lower incomes and contend with other social and health disadvantages, including reduced access to care.
- Among American Indians, rates of diabetes are 2 to 5 times higher than those of Whites, and Mexican Americans and Puerto Ricans are twice as likely to develop the disease than non-Hispanic Whites of similar age.
- African American adults, on average, are 1.7 times more likely to develop diabetes than Whites, while the majority of children and adolescents with Type 2 diabetes are people of color.
- In the Appalachian Region and Deep South, socioeconomic conditions, lifestyle, and culture have combined to create the Diabetes Belt, a 644-county area in 15 states with substantially higher rates of Type 2 diabetes.
Diabetes: A population health problem
The root cause of diabetes isn’t known, but factors such as obesity, poor diet, and physical inactivity greatly increase the risk of developing the disease or its precursors. Those with lower incomes may face chronic food insecurity and often lack access to a nutrient-rich diet.
Combined with low health literacy, this can result in diets of calorie-dense, high-fat foods, which cost less and may be easier to obtain than fresh vegetables and fruit. Over time, low-quality diets can set the stage for reduced physical activity, obesity, prediabetes and ultimately, the onset of the disease.
Prevention is key to diabetes population health strategies
Reversing the disease’s rampage through the America’s most disenfranchised populations hinges on dramatic improvements in prevention.
Better prediabetes screening and treatment are essential: One recent study examining more than 20,000 electronic health records found that of the 63% of patients screened for prediabetes, 26% were found to be potentially at risk for the disease. Yet of that group, only 5% were subsequently diagnosed with prediabetes and none received appropriate treatment for the condition.
Social, economic disparities foster diabetes root causes
More fundamentally, effective diabetes prevention requires tackling the complex, intertwined social determinants of health (SDoH) that elevate risk in the first place. The graphic below shows the five broad categories of social determinants.
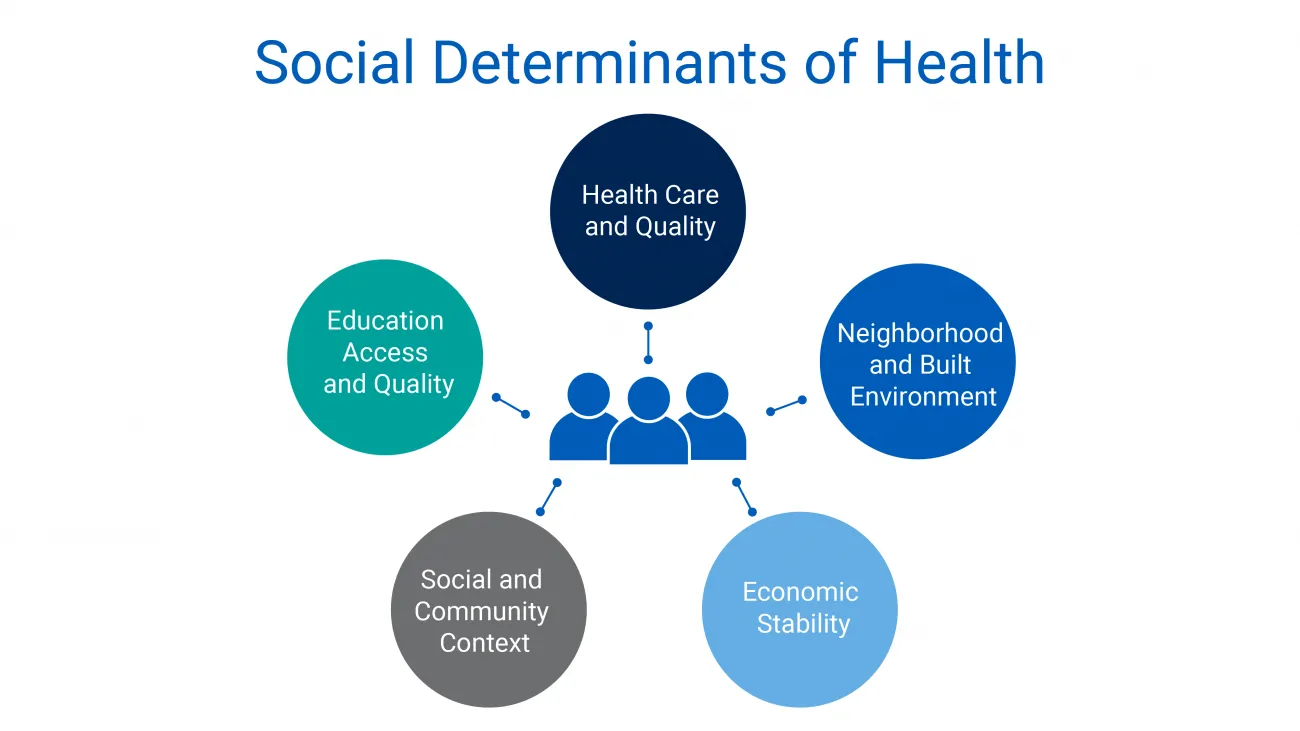
According to the Centers for Disease Control (CDC) 13% of U.S. adults with less than a high school education have diabetes, versus just 7% among those with a greater than a high school education. Lower education levels contribute to low health literacy and can also result in poor medication adherence among patients who are prescribed insulin to control the disease.
Compounding these risks are the grinding life conditions many lower-income people face day-to-day, from poor income and employment opportunities and food insecurity to housing instability, sporadic transportation, and domestic or neighborhood violence.
Combined with lower levels of health coverage, limited access to care, and medical mistrust, social determinants heighten the chances a person will develop diabetes and increase the odds the disease will remain undiagnosed and untreated.
Change efforts must support population health
Despite the rising incidence of diabetes, there’s encouraging news. Efforts are ramping up on multiple levels to address SDoH that contribute to the illness. Examples of diabetes population health strategy initiatives include:
The federal government’s Healthy People 2030 initiative has created a framework for decreasing diabetes incidence and improving treatment by, among other things, increasing patient access to diabetes education and boosting the number of adults who monitor their blood sugar daily.
CDC has developed a comprehensive diabetes prevention program that providers can implement to help their patients make better diet and lifestyle choices.
The American Diabetes Association has developed a broad set of recommendations for addressing SDoH, including establishing consensus around SDoH definitions and metrics, prioritizing research to target social determinants, helping ensure SDoH considerations are embedded in research and evaluation studies, and training researchers to assess the impact of next-generation SDOH interventions.
Payers and providers are playing a critical role in showing the tangible, often dramatic benefits realized by addressing social determinants. Case in point: A program implemented by Geisinger Health System includes 15 hours of education about diabetes and healthy living and 10 free meals weekly. Program results show an 80% reduction in annual diabetic care costs, down from $240,000 per patient to $48,000.
A collective commitment to prevention
Given the enormous costs in both lives and resources diabetes has already extracted, its alarming growth trajectory, and the entrenched factors that continue to accelerate its progress, attempts to reverse the tide may seem like too little, too late. But with prevention’s value self-evident, it’s incumbent upon the healthcare system to implement effective and sustainable methods to stop diabetes before it has a chance to develop.
Starting is the first step on the road to success
In recognizing the underlying social and economic conditions that affect health literacy and access to care, we can develop effective community-based programs to better inform behaviors, connect people with resources, improve access to care, and institute interventions that support patients with high-risk profiles for diabetes.
There’s much still to be done to close the health equity gap. But these and other actions can slow the epidemic, minimize health inequities, contain treatment costs, and contribute to better health outcomes.
Learn more about RTI Health Advance’s population health solutions.
Subscribe Now
Stay up-to-date on our latest thinking. Subscribe to receive blog updates via email.
By submitting this form, I consent to use of my personal information in accordance with the Privacy Policy.