We've joined our RTI Health Solutions colleagues under the RTI Health Solutions brand to offer an expanded set of research and consulting services.
Addressing social drivers or determinants of health (SDoH) has become a top priority for public and private institutions. A growing commitment to addressing long-standing disparities in health outcomes caused by social drivers of health has accelerated the development of data measures, scores, and indices. Conceptualizing and measuring social drivers of health, health-related social needs (HRSN), and social risk factors (SRF) are key to creating national or state policies and payment regulations and improving population health. These steps pave the way for payers, providers, communities, and researchers to understand the impact of social drivers and health inequity on the people and populations living and working within the institutions' respective areas of influence.
Making sense of a plethora of social drivers or determinants of health
There is an enormous number of SDoH- and health equity-related indices, indicators, measures, and scores in the field. Some estimate the number reaches the hundreds.
Because there are so many indices, the HHS Office of the Assistant Secretary for Planning and Evaluation (ASPE) commissioned the RAND Corporation to conduct a review and provide recommendations. Released in September 2022, the report's goal was to recommend which index would be best for CMS's purposes: determining Medicare payment policies that provide resources and incentives to providers for screening and addressing SDoH. RAND's review encompassed 21 measures.
Published in December 2022, RTI International reviewed SDoH indices, creating an in-depth study of the 6 most commonly used. Also published in December 2022, a team of researchers completed a scoping and qualitative analysis of socioeconomic deprivation indices in Health Affairs, reviewing 15 indices. And yet, a review for this article found another 10-plus indices in the space, revealing how deciding on an index provides an overwhelming number of choices.
Figure 1 provides a sampling of SDoH and health equity indices available.
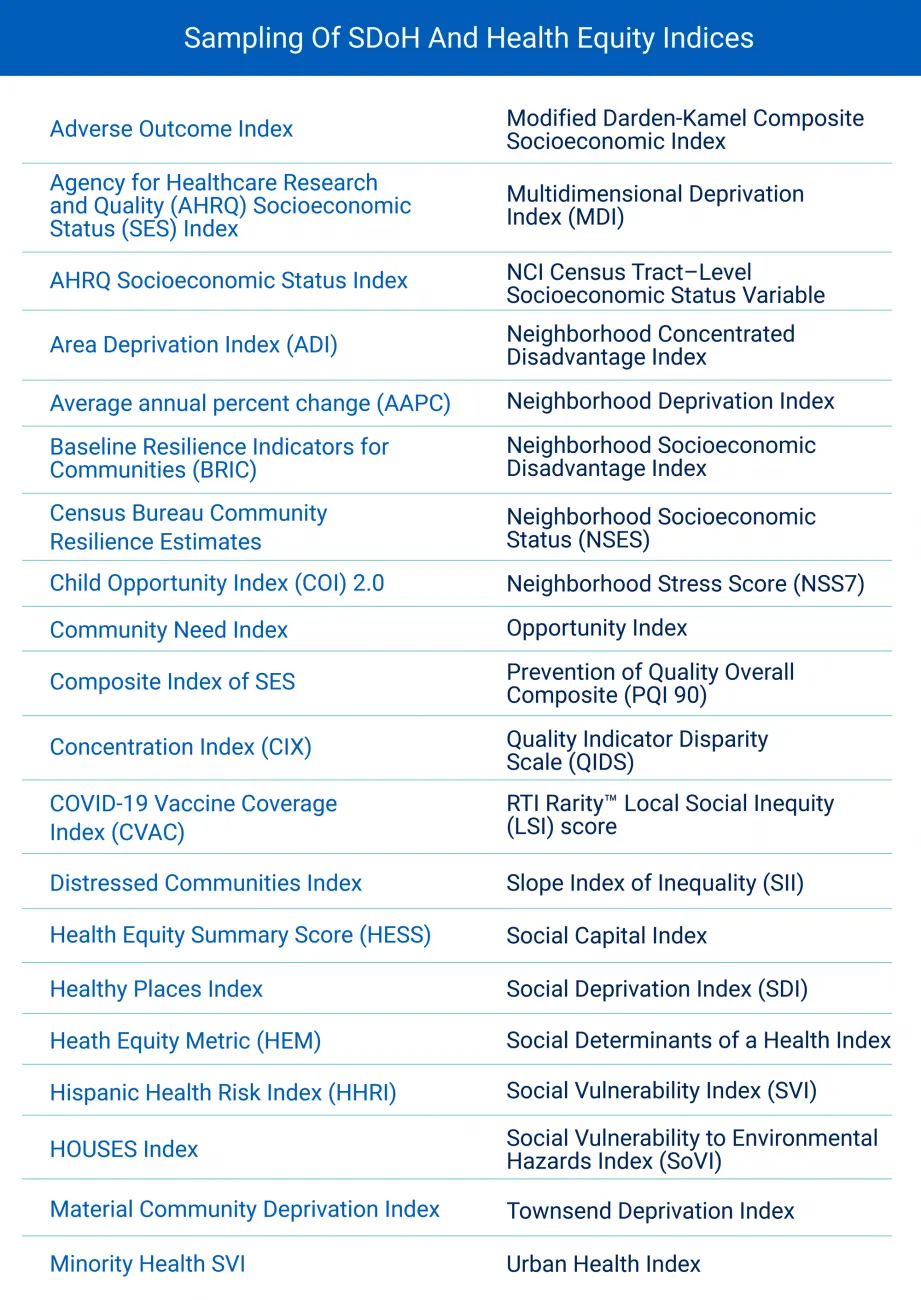
Figure 1: Sampling of SDoH and Health Equity Indices
SDoH and health equity primer for choosing the right health index
With so many indices available and so few comparative analyses (qualitative or quantitative), how can a healthcare or public health professional select the best option for their needs? Our review provides a primer to SDoH and health equity indices, creating a foundation from curated research and work in the field, ending with questions to ask when vetting an index.
SDoH or health index definitions and foundational concepts
There are primarily 2 types of health data indices covering many issues and themes across social drivers of health. Some are used for ranking and recognition, some for data analysis and research, and others serve both purposes.
For example, the Health Equality Index (HEI) measures and ranks over 2,200 healthcare facilities nationwide on LGBTQ+ inclusion. HEI is a benchmarking tool that evaluates healthcare facilities' policies and practices. In the second category are indices like the Area Deprivation Index (ADI) that share measures of neighborhood disadvantage with the public, including educational institutions, health systems, not-for-profit organizations, and government agencies, to make these metrics available for use in research, program planning, and policy development. The Neighborhood Atlas website allows the mapping of ADI data as well as the ability to download rankings.
Key definitions and social risk categories
It's pivotal to anchor any review of health indices in definitions of the themes covered. The method by which a health index defines key concepts will significantly influence how it is created and the type and source of information it will serve.
The following definitions are widely accepted and provide a foundation for health index analysis and discussion:
- Social determinants of health (SDoH - aka social drivers of health): As defined by the World Health Organization (WHO) and adopted by the Centers for Disease Control and Prevention (CDC), SDoH are nonmedical factors that influence health outcomes. They are the conditions in which people are born, grow, work, live, and age, and the wider set of forces and systems shaping the conditions of daily life. These forces include economic policies and systems, development agendas, social norms, social policies, racism, climate change, and political systems.
- Social risk factors (SRF): An individual-level attribute or lived experience resulting from an adverse SDoH that increases the likelihood of poor health.
- Health-related social needs (HRSN): Individual-level consequences of social and economic conditions (SDoH and SRF) that affect a person's ability to maintain their health and well-being. HRSN arise from unmet social need including: housing instability; poor quality housing; food insecurity; unemployment and underemployment; unsafe communities, homes, and interpersonal violence; lack of transportation; and unaffordable utilities.
- Health equity: According to the WHO, "Health equity is achieved when everyone can attain their full potential for health and well-being." It's achieved when equity in healthcare is attained. "Equity is the absence of unfair, avoidable or remediable differences among groups of people, whether those groups are defined socially, economically, demographically, or geographically or by other dimensions of inequality (e.g., sex, gender, ethnicity, disability, or sexual orientation).
With these definitions in mind, at the highest level, an index focuses on 1 or more of the following 6 social risk areas as outlined in the 2022 report prepared for ASPE, Landscape of Area-Level Deprivation Measures and Other Approaches to Account for Social Risk and Social Determinants of Health in Health Care Payments:
- Socioeconomic position: income or wealth, education, occupation
- Race, ethnicity, and cultural context: race/ethnicity, language, nativity, acculturation
- Gender: gender, gender identity, sexual orientation
- Social relationships: marital status, social support
- Residential and community context: community socioeconomic composition, built environment
- Social needs: housing instability, food insecurity, interpersonal safety
SDoH and health equity indices can provide a broader perspective
According to the Organization for Economic Co-operation and Development (OECD), an index is "a composite indicator that is formed when individual indicators are compiled into a single index, based on an underlying model of the multi-dimensional concept that is being measured."
Further, a summary index integrates performance on multiple quality targets and may incorporate multiple domains of social risk. For example, CMS's Office of Minority Health (OMH) created the Health Equity Summary Score (HESS) by integrating multiple clinical and patient-experience quality measures to benchmark performance and improvement across race, ethnicity, and socioeconomic status. When the technical expert panel RAND convened for their analysis, the HESS score received the highest ranking as a composite index.
Understanding the nature of a health index will support an evaluator's decision about whether an index is the most appropriate data form for their analysis or research needs.
Value and purpose of SDoH and health equity indices
A SDoH or health equity index can provide enormous value, insight, and efficiency to achieve a health equity and population health aim. Once the index is fully understood, analysts and decision makers can have confidence in their foundational research, achieve greater multi-stakeholder support, and accelerate action to launch programs and policies.
For example, America's Health Insurance Plans (AHIP) reported that many health plans are "identifying at-risk populations, designing programs based on member needs, and mapping and cataloguing existing community resources." Indices provide the collective data to create, launch, and measure such initiatives.
How indices are used–case examples
Real-world cases demonstrate the variety and value of many healthcare-related entities that derive from SDoH and health equity indices. Here are 4 examples:
- CMS incorporated SRF into Medicare payments to providers. Most recently, they proposed increased payments to new ACOs that care for dually eligible beneficiaries who live in areas with high deprivation by utilizing the Area Deprivation Index (ADI).
- The Healthy Places Index (HPI) was used in California during the COVID-19 pandemic to direct $272 million in federal COVID funding to disproportionately impacted communities.
- Humana created an overall social risk index to feed data into its main clinical risk model. The company pulls social risk data from internal, community, and consumer sources, using the information for predictive analysis, prioritizing member outreach, and addressing beneficiary social needs.
- Ohio Medicaid piloted the RTI RarityTM score to identify the 5 most important predictors of shorter life expectancy by utilizing more than 140 publicly available variables specific to the state. With this index, the organization uncovered 10-20% more variability in life expectancy.
These examples scratch the surface of how SDoH and health equity indices are being used by government and public health departments, state Medicaid and MCOs, payers, and providers. Whether selecting a new index or reassessing past index choices, it's vital to ask and answer strategic questions to uncover the one that will best meet the current need.
Which index meets your SDoH, health equity, and public or population health objectives?
An evaluation framework can help uncover the critical characteristics of an index. The use of such a framework can ensure that any choice is transparent and meets stated analytical or programmatic goals.
A series of structured questions can help reveal features of indices, allowing them to be ranked according to alignment with organizational priorities.
Health index characteristics for vetting
These 8 health index characteristics can be used by data scientists as an essential checklist or to highlight aspects of indices when presenting recommendations to leadership and stakeholders. These characteristics are particularly helpful when comparing and contrasting indices.
- Input domains and domain definitions
- Index statistical approach and data transformation
- Geography and level of granularity
- Data sources and input variables
- Accessibility
- Output types and measures
- Index oversight and governance
- Advanced technologies
Health index vetting questions by characteristic area
The following 8 areas include examples of questions that can be used to uncover index features and rank order before recommending or choosing the best index to meet current or future needs.
1. Input domains and domain definitions
Typically, an index would cover 1 or more of the 6 social risk domains listed earlier. For example, "social context" is a domain, and demographics, age, race/ethnicity, social vulnerability index, segregation, and living conditions are all sub-domains. How an index creator defines the domains is essential to ensure that the focus of the index and its foundational data sources align with the index use case.
- Is there a goal or creation statement for this index describing its objective?
- Are domains and any sub-domains defined?
- Why was this index created?
2. Index statistical approach and data transformation
Consider the methodical approaches used to create the index, including the use of empirical findings, theory, or both, as well as how the included index variables were chosen. Data transformation refers to the statistical methods used to break down many variables into fewer variables, such as, factor loading or principal component analysis and whether the data are stratified, normalized, or standardized.
- Which statistical methodologies were used in creating this index?
- Were multiple imputations of missing demographic characteristics performed to complete datasets?
- Was a random forest model used?
- Was principal component analysis, summation, or averaged values used?
- How was predictive modeling used?
3. Geography and level of granularity
Geography entails what geographical unit the index covers or has been applied–country, state, county, city, community, etc. Granularity is also a consideration of geography when determining if an index uses data at the census-tract level, area level, or individual level.
- What is your ideal level of geographic disaggregation?
- Do you need census-tract or census block-group levels, or do you require different geographic areas or flexibilities?
- What compromises are you able to make for more granularity?
4. Data sources and input variables
Input variables encompass the number of measures or dimensions included, how new the data are, how many data points or measures were used, and their source's validity.
- How many input variables were used?
- What is the external validity of those inputs?
- Can variables be broken down into subcategories?
- What is the data lag and how often is the baseline data updated?
- Can original data sources be confirmed or validated, if needed?
5. Accessibility
This characteristic includes whether an index is publicly available or a commercial index that's only used within an organization or externally for a fee. It also includes whether an index was pre-created, without the need to compute input variables, or if the data required was transformed in some way.
- Is there a fee required to access the data?
- If an index wasn't chosen, what is the time cost to create or tailor an index internally or with an outside firm?
6. Output types and measures
Covering the nature of the data output garnered from the index, output types and measures can include a ranking or score.
- Does this index provide a ranking/score, or does it also provide data that can be used for further analysis and transformation?
- What is the type of output that this index offers?
- Does the creator provide access to an online visualization tool only?
- Can you access or download the raw data or data reports from the index?
- What other data visualizations, reports, or output does this index offer?
7. Index oversight and governance
Index oversight and governance includes who created the index and their capabilities to do so, who maintains the index, as well as how measures were vetted for inclusion–through expert panels, outside consultants, or other subject matter review.
- Who published the index?
- Who carried out the index creation and design?
- Did an expert panel review the index before it was published? Or was the index externally validated in some other way?
- Is there any information about who is using this index now and how it is being used?
- How is the index governed or updated over time?
- Are users of the index able to provide feedback?
8. Advanced technologies
Advanced technologies entail any artificial intelligence (AI) or machine-learning (ML) technologies used to create associations among measures or used as part of reduction or clustering algorithms or data processing automation.
- Were advanced technologies–like AI/ML–applied to the data? If so, in what ways?
- Was the data transformed using techniques like reduction, clustering algorithms, or automation?
Ensuring an index aligns with SDoH and health equity objectives
Ultimately, an index must align with the program's SDoH and health equity objectives. The authors of the Health Affairs article on area-based socioeconomic deprivation indices offer wisdom to this end, "Developing an understanding of the key characteristics of each index, and the variability between indices, is an important step for public health practitioners and health outcome researchers to take before index selection and application."
Use an index or create your own through custom data analytics, reports, and dashboards
Choosing the most appropriate and robust SDoH or health equity index to meet your current or future needs is daunting. RTI Health Advance has health equity, data science, population health, and public health experts to support your decision. We also offer our RTI Rarity Local Social Inequity (LSI) score that merges artificial intelligence, advanced data science methods, and geospatial analytics in a risk adjustment framework.
Learn more or contact us.
Subscribe Now
Stay up-to-date on our latest thinking. Subscribe to receive blog updates via email.
By submitting this form, I consent to use of my personal information in accordance with the Privacy Policy.